Accessing the vasa can be achieved with a single or double incision to the scrotum using a scalpel or with the no-scalpel technique using special instruments. No-scalpel vasectomy has been shown to reduce the risk of complications (i.e., bleeding and infection) compared with the incision technique [4].
Technique options can be divided into three components of vasectomy: acceding the vasa, disrupting the vasa and closing the surgical site. Disruption of the vasa can be performed in numerous ways. Simple suture ligation with excision likely is the most common method worldwide, although this method has been shown to be less effective [5-6]. It is recommended the no-scalpel approach using vas division with fascial interposition or intraluminal diathermy since this method has lower short-term complications with a higher success rate as compared to the incision technique without the above measures [7-8].
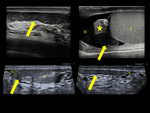
By ultrasound, we can appreciate changes in the epididymis. A statistically significant difference in the incidence of thickened epididymis (those with a head thicker than 1.5 cm and a body and tail thicker than 0.5 cm) was found between the vasectomy and nonvasectomy groups [9]. Epididymal tubules are not normally seen on sonograms. It is defined as tubular ectasia when these tubules became visible. This sonographic sign is defined as a variable degree of enlargement of the epididymal body with multiple interfaces between the epididymal tubule wall and fluid which gives it a hypoechogenic appearance. In such patients, the tail and occasionally the head of the epididymis are also involved. On color Doppler sonography, tubular ectasia of the epididymis is typically hypovascular. A significantly higher incidence of epididymal tubular ectasia was found in the vasectomy group than in the control group [9] but can be also seen with other causes of obstruction of the ductus deferens. (Fig. 1)
Complications following vasectomy include hematoma, infection, sperm granuloma and testicular necrosis.
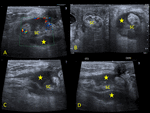
Hematoma formation is a common complication associated with vasectomy with an incidence of about 2% (range, 0.09-29%) [10]. The most common site of bleeding is the pampiniform plexus of veins. Hematoma rates are lower for no-scalpel procedures, where tissue dissection is minimized [10]. (Fig. 2). The US appearance of extratesticular hematoceles varies with their age. Acute hematoceles are echogenic in appearance, whereas chronic hematoceles tend to become anechoic over time and develop septa and loculations that may show internal fluid-fluid levels and faint echoes.
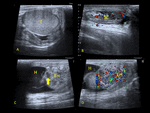
The incidence of infection varies between 0.3–38%, with an average of about 3.4% [11-12]. This includes wound, urinary, funiculitis and epididymitis. (Fig. 3) Hematoma formation, as well as pre-operative positive semen and urine cultures, are reported risk factors [12]. The epididymal tail is the most affected region, and reactive hydrocele and scrotal wall thickening are frequently present. On US increased size and, depending on the time of evolution, decreased, increased, or heterogeneous echogenicity of the affected organ are usually observed. In funiculitis, we can appreciate that the spermatic cord is thickened and more echogenic than normal with increased vascularity.
Sperm cell granuloma is considered a form of chronic epididymitis which occurs secondary to inflammation, trauma, and/or a vasectomy. A granulomatous reaction forms secondary to extravasated sperm cells. On US it can appear as a well-circumscribed heterogeneous mass and are commonly found at the epididymis or the ends of the divided ductus deferens.
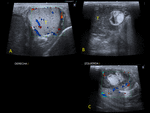
Testicular necrosis is less frequent but we also need to know how to identify it. (Fig. 4). A heterogenous testis with lack of flow on color
/power Doppler suggests testicular ischemia or infarct. During vasectomy, it is important to dissect the bare vas to minimize vascular injury [13].